Flexible Spending Accounts (FSA)
Brown & Brown and Hawaii Teammates
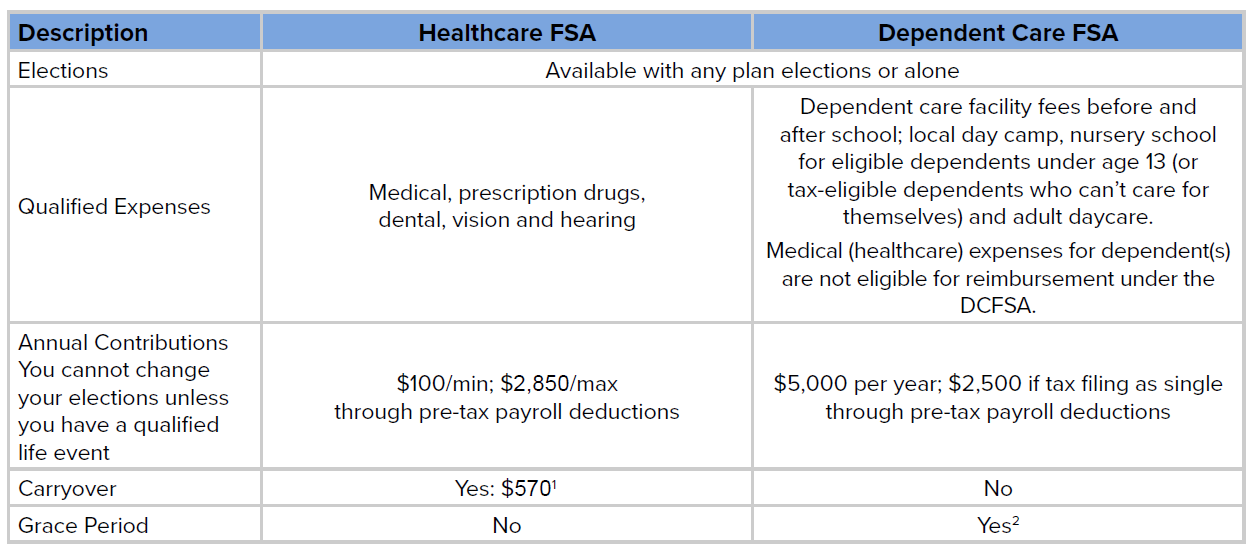
Brown & Brown provides you with the opportunity to pay for eligible un-reimbursed medical, dental, vision and dependent care expenses on a pre-tax basis.
Administrative services and claim reimbursements for Healthcare FSA (FSA) and Dependent Care FSA (DCFSA) are provided by HealthEquity/WageWorks.
- Debit cards for dependent care elections are not issued by HealthEquity/WageWorks. Expenses for reimbursement can be submitted through the member portal on the HealthEquity/WageWorks website, completion of a DCFSA reimbursement form or through the HealthEquity/WageWorks mobile app. Recurring DCFSA claims can be scheduled for the duration of the Plan Year. Reimbursements will be made through direct deposit to an account specified by you.
- The Flex Plan Year is January through December. Eligible expenses must be incurred by December 31st to be qualified for reimbursement in the current Plan Year. The Healthcare FSA does include a carryover provision and the DCFSA includes a 2.5 month grace period. Eligible expenses incurred during the Flex Plan Year must be submitted by the following March 31st. It is important to choose your annual amount(s) carefully to avoid any unused funds at the close of the Plan Year.
- Healthcare FSA can be reimbursed up to the total amount you have elected to deposit for the year. If termination of the Healthcare FSA occurs prior to the end of the Plan Year, you are only eligible for reimbursement of expenses which were incurred while you are a participant in the Plan unless (if applicable) COBRA continuation is elected.
- Dependent Care can be reimbursed up to the total amount you have deposited. If termination of the DCFSA occurs prior to the end of the Plan Year, you can continue to request eligible reimbursements until the earlier of the date your balance is exhausted or the end of the Plan Year.
- New elections are required for your Healthcare FSA and/or DCFSA. If you do not make new elections for 2022, your participation in these accounts will end. Elections do not roll-over from year to year.
1Current plan participants with funds remaining in your FSA as of 12/31/21 will have up to $570 of those unused funds carry over and can be used for eligible expenses incurred in 2022. Any unused funds over and above $570 will be forfeited. For example, if you contributed $2,750 to the FSA in 2021 and only incurred eligible expenses totaling $2,000, $570 would carry over into 2022 but the remaining $180 of unused funds would be forfeited.
2Current plan participants with funds remaining in your dependent care account as of 12/31/21, a 2.5 month grace period, January 1 – March 15, will allow for additional time to spend those dollars. You will have until March 15, 2022 to incur eligible dependent care expenses and use money left over from 2020 to pay them. The last day to submit claims is March 31, 2022. Any unused funds would be forfeited after the grace period ends.
Note: Employees are required to follow all tax laws and are encouraged to consult with your tax professional with questions or need assistance with your FSA enrollment.
IMPORTANT DOCUMENTS:
Proctor Loan Protector Teammates
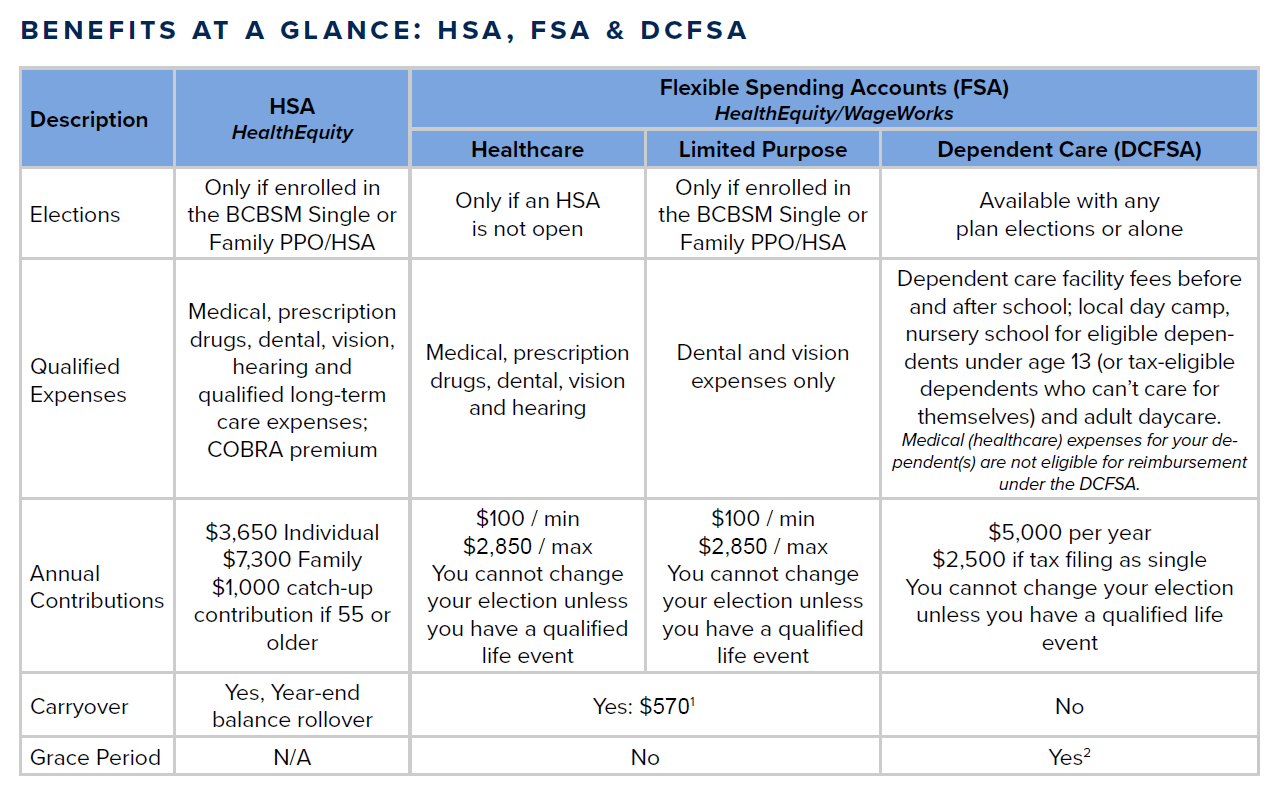
Brown & Brown provides you with the opportunity to pay for unreimbursed medical, dental, vision, and dependent care expenses on a pre-tax basis. Administrative services and claim reimbursements for Healthcare FSA, Limited Purpose FSA and Dependent Care FSA (DCFSA) are provided by HealthEquity/WageWorks).
- New HealthEquity FSA debit cards will be issued for new enrollees.
- The HealthEquity Healthcare card cannot be used for eligible dependent care expenses. Expenses for DCFSA reimbursement can be submitted through the member portal on the HealthEquity/WageWorks website, completion of a DCFSA reimbursement form or through the HealthEquity/WageWorks mobile app. Recurring DCFSA claims can be scheduled for the duration of the plan year. Reimbursements will be made through direct deposit to an account specified by you.
- The Flex Plan Year is January through December. Eligible expenses must be incurred by December 31st to be qualified for reimbursement in the current plan. Both the Healthcare and Limited Purpose FSA include a carryover provision and the DCFSA includes a 2.5 month grace period. Eligible expenses incurred during the Flex Plan Year must be submitted by the following March 31st. It is important to choose your annual amount(s) carefully to avoid any unused funds at the close of the Plan Year.
- Healthcare and Limited Purpose FSA can be reimbursed up to the total amount you have elected to deposit for the year. If termination of either FSA occurs prior to the end of the plan year, you are only eligible for reimbursement of expenses which were incurred while you are a participant in the Plan unless (if applicable) COBRA continuation is elected.
- Dependent Care can be reimbursed up to the total amount you have deposited. If termination of the DCFSA occurs prior to the end of the Plan Year, you can continue to request eligible reimbursements until the earlier of the date your balance is exhausted or the end of the Plan Year.
1Current plan participants with funds remaining in your FSA as of 12/31/21 will have up to $570 of those unused funds carry over and can be used for eligible expenses incurred in 2022. Any unused funds over and above $570 will be forfeited. For example, if you contributed $2,750 to the FSA in 2021 and only incurred eligible expenses totaling $2,000, $570 would carry over into 2022 but the remaining $180 of unused funds would be forfeited.
2Current plan participants with funds remaining in your dependent care account as of 12/31/21, a 2.5 month grace period, January 1 – March 15, will allow for additional time to spend those dollars. You will have until March 15, 2022 to incur eligible dependent care expenses and use money left over from 2021 to pay them. The last day to submit claims is March 31, 2022. Any unused funds would be forfeited after the grace period ends.
Note: Employees are required to follow all tax laws and are encouraged to consult with your tax professional with questions or need assistance with your FSA enrollment.
IMPORTANT DOCUMENTS:
Health Savings Accounts (H.S.A.)
Brown & Brown Teammates
Brown & Brown will continue in 2022 to pay HSA maintenance administrator fees for active teammates with an Optum Bank HSA account.
Optum HSA Customer Service
Phone: The customer support center is available for assistance from 7 a.m. to 7 p.m. (Central Time), Monday through Friday at (800) 791-9361.
Email: [email protected]
Download the Optum Bank mobile app to view your account info
Proctor Loan Protector Teammates
- Available when enrolled in the BlueCross Blue Shield of Michigan (BCBSM) PPO/HSA Plan.
- HealthEquity is the NEW HSA provider effective January 1, 2022 and is fully integrated with BCBSM. You will be able to manage your HSA through the BCBSM portal at bcbsm.com or on the BCBSM mobile app after January 1, 2022.
- Visit HealthEquity’s HSA webpage for tools, forms and information on the HealthEquity HSA.
- HSA 2022 contribution limits: Individual=$3,650; Family=$7,300; $1,000 catch-up contribution for age 55 or older participants.
IMPORTANT DOCUMENTS:
NOTE: You may be disqualified from any tax advantages of a contribution to a Health Savings Account (HSA) if you (or any of your covered eligible dependents) are enrolled in another health benefit plan while covered by a qualified HDHP with a HSA. Your participation in a Healthcare FSA (either through Brown & Brown or through your eligible dependent) is considered as another plan. This notice is not meant to be considered legal or tax advice. Employees are required to follow all tax laws and are encouraged to consult with your tax professional with questions or need assistance with your FSA and/or HSA enrollment.